Diet Guide to Prepare for Immunotherapy
As cancer patients prepare to come to Cancun to begin their personalized Immunotherapy journey, they often ask if there are things they can do to “improve the odds of success.” And while there are a few things, the focus here will be on diet and how it could improve the response of the Immunocine Therapy.
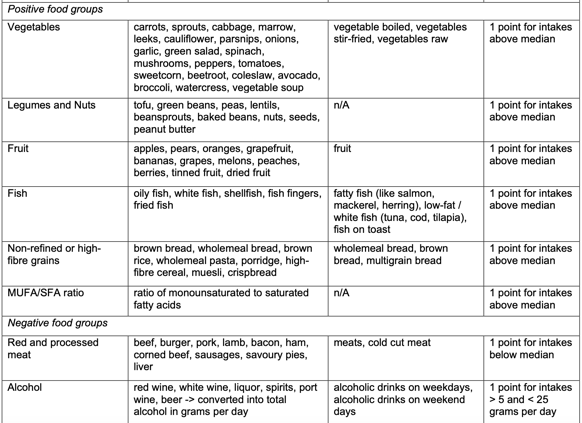
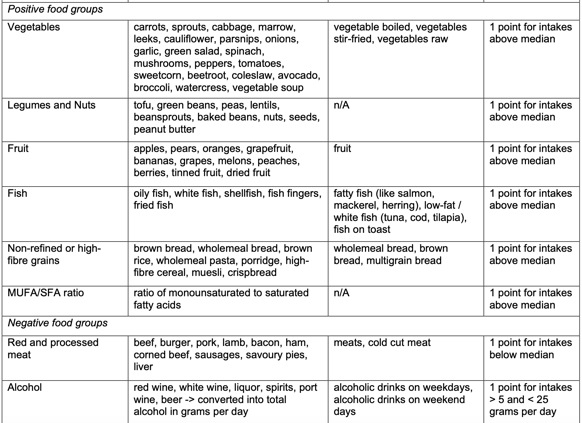
Recently Jama Oncology published a study in which 91 melanoma patients were retrospectively stratified based on their diets and responses to non-specific Immunotherapy were concurrently analyzed1.
Types of Immunotherapy Friendly Diets
Though the specifics of their algorithm are less important at this juncture, the take away was that there was a positive correlation between adherence to a Mediterranean Diet (containing mono and polyunsaturated fats from olive oil, nuts, and fish; polyphenols; and fiber from vegetables, fruit, and whole grains, lean meat, whole eggs, dried lentils, peas, and beans, limited red meat and dairy) and objective response measures (such as progression free survival (PFS) and overall survival (OS) when on immunotherapy for cancer.
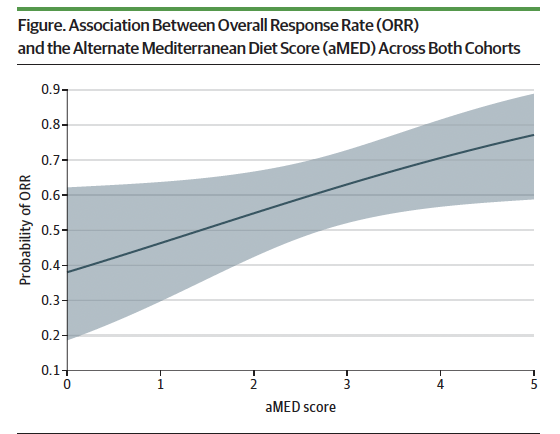
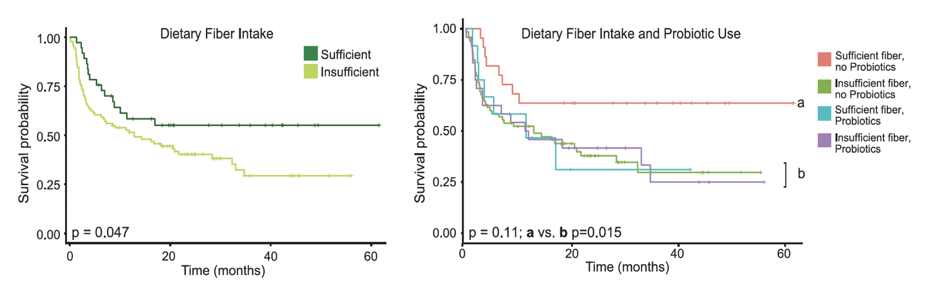
This falls in line with another recent publication in Science that demonstrated a robust improvement to immunotherapy if >20g of dietary fiber were consumed each day2.
Importance of Fiber on a Cancer Friendly Diet
It has been known for a while that sufficient dietary fiber can reduce the odds of developing cancer3, 4, and improve survival post a cancer diagnosis5, 6, but this was one of the first studies to show a strong correlative link between dietary fiber and immunotherapy’s ability to assist a patient in overcoming their cancer2.
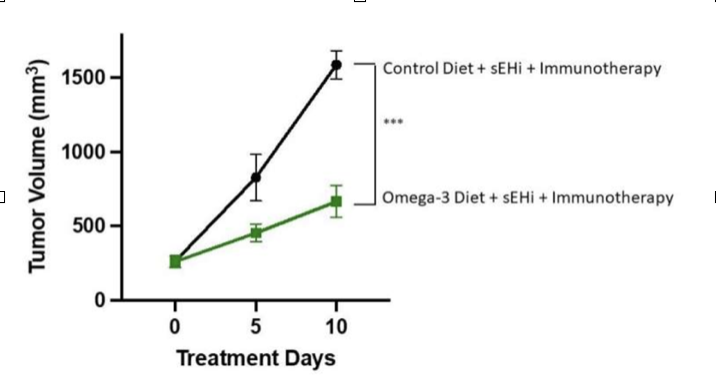
A study in Nature Medicine echoed these results7 and added to them by finding that “…response rates were higher in Ruminococcaceae-dominated microbiomes than in Bacteroidaceae-dominated microbiomes…Poor response was associated with lower fiber and omega 3 fatty acid consumption…” This fits with some other studies that have shown a modest protection against cancer when consuming Vitamin D3 and Omega-3’s8, 9, but better still that Omega-3’s may reduce cancer-driven immunosuppression allowing for stronger immunotherapy results10, 11.
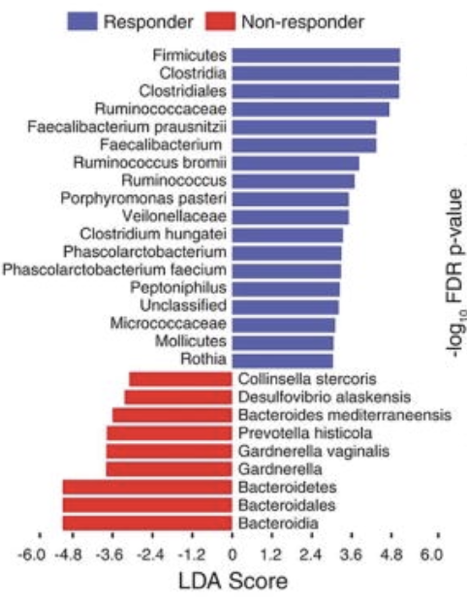
Additionally, some microbiota have been found to enhance responsiveness to Immuno-therapy12. For example, it was demonstrated that there is a statistically significant positive correlation between the CD8+ T cell infiltrate in the tumor and abundance of the Faecalibacterium genus, the Ruminococcaceae family and the Clostridiales in the gut and a non-significant but negative correlation with Bacteroidales13, 14.
Though studies continue, there is evidence that a there is a food-gut axis relevant to cancer immunotherapy15.
They found that patients most likely to respond to immunotherapy are those who have both “beneficial” bacteria and a fiber-rich, plant-based diet needed to feed those bacteria.
And just as important is what not to eat. Though not all mechanisms are fully understood yet, hyperglycemic diets have been shown to accelerate tumor growth and aggressiveness and are best to be avoided during this time16, 17.
Hyperglycemia is defined by an elevated glucose level in blood plasma (>125 mg/dL while fasting and >180 mg/dL 2 h after eating)18 and has been associated with metabolic and molecular alterations that promote cancer growth and aggressiveness19, 20.
None of this is to say that there is a magical diet that will rid the body of advanced cancer, nor is it to say that eating a cupcake will doom a patient. These extremes have not been demonstrated to be true, and stressing about this (which increase stress hormones that also promote cancer growth21, 22) is not beneficial or necessary.
However, within the data subsets, it begins to become apparent that there are a couple of themes that a cancer patient could take to heart when considering how to fuel their body to slow cancer growth and empower the immune system.
5 Ways to Eat Healthy Pre Immunotherapy Treatment (and in general)
Even just incorporating the following 5 dietary suggestions could bring about a hefty, life-altering, return.
Mostly avoid red meat, simple carbohydrates, and hyperglycemic foods and drinks.
Add fruits and vegetables to your diet; considerably.
Turn to fish and nuts as a good source of protein and oil that will be beneficial.
No reason to be boring; add some spice that has shown benefit in strengthening the immune system.
Add beans, peas, and lentils to increase your dietary fiber to above 20g/day.
References
1. Bolte, L.A. et al. Association of a Mediterranean Diet With Outcomes for Patients Treated With Immune Checkpoint Blockade for Advanced Melanoma. JAMA Oncol (2023).
2. Spencer, C.N. et al. Dietary fiber and probiotics influence the gut microbiome and melanoma immunotherapy response. Science 374,1632-1640 (2021).
3. Kunzmann, A.T. et al. Dietary fiber intake and risk of colorectal cancer and incident and recurrent adenoma in the Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial. Am J Clin Nutr 102,881-890 (2015).
4. McRae, M.P. The Benefits of Dietary Fiber Intake on Reducing the Risk of Cancer: An Umbrella Review of Meta-analyses. J Chiropr Med 17,90-96 (2018).
5. Song, M. et al. Fiber Intake and Survival After Colorectal Cancer Diagnosis. JAMA Oncol 4,71-79 (2018).
6. Zhao, J. et al. Association between Dietary Fiber Intake and Mortality among Colorectal Cancer Survivors: Results from the Newfoundland Familial Colorectal Cancer Cohort Study and a Meta-Analysis of Prospective Studies. Cancers (Basel) 14 (2022).
7. Simpson, R.C. et al. Diet-driven microbial ecology underpins associations between cancer immunotherapy outcomes and the gut microbiome. Nat Med 28,2344-2352 (2022).
8. Bischoff-Ferrari, H.A. et al. Combined Vitamin D, Omega-3 Fatty Acids, and a Simple Home Exercise Program May Reduce Cancer Risk Among Active Adults Aged 70 and Older: A Randomized Clinical Trial. Front Aging 3,852643 (2022).
9. Nindrea, R.D., Aryandono, T., Lazuardi, L. & Dwiprahasto, I. Protective Effect of Omega-3 Fatty Acids in Fish Consumption Against Breast Cancer in Asian Patients: A Meta-Analysis. Asian Pac J Cancer Prev 20,327-332 (2019).
10. Zhang, H. et al. Docosahexaenoic acid reverses PD-L1-mediated immune suppression by accelerating its ubiquitin-proteasome degradation. J Nutr Biochem 112,109186 (2023).
11. Zhao, H. et al. Fish consumption in multiple health outcomes: an umbrella review of meta-analyses of observational and clinical studies. Ann Transl Med 11,152 (2023).
12. Oh, B. et al. The Gut Microbiome and Cancer Immunotherapy: Can We Use the Gut Microbiome as a Predictive Biomarker for Clinical Response in Cancer Immunotherapy? Cancers (Basel) 13 (2021).
13. Gopalakrishnan, V. et al. Gut microbiome modulates response to anti-PD-1 immunotherapy in melanoma patients. Science 359,97-103 (2018).
14. Wu, J. et al. Modulation of Gut Microbiota to Enhance Effect of Checkpoint Inhibitor Immunotherapy. Front Immunol 12,669150 (2021).
15. Russo, E., ; Nannini, G,; Dina, M,; Pagliai, G,; Sofi, F,; Amedei, A. Exploring the food-gut axis in immunotherapy response of cancer patients. World J Gastroenterol. 7,4919-4932 (2020).
16. Li, W. et al. Effects of hyperglycemia on the progression of tumor diseases. J Exp Clin Cancer Res 38,327 (2019).
17. Phoomak, C. et al. High glucose levels boost the aggressiveness of highly metastatic cholangiocarcinoma cells via O-GlcNAcylation. Sci Rep 7,43842 (2017).
18. Mouri, M. & Badireddy, M. Hyperglycemia. StatPearls: Treasure Island (FL), 2022.
19. Ramteke, P., Deb, A., Shepal, V. & Bhat, M.K. Hyperglycemia Associated Metabolic and Molecular Alterations in Cancer Risk, Progression, Treatment, and Mortality. Cancers (Basel) 11 (2019).
20. Gahler, A. et al. Glucose-Restricted Diet Regulates the Tumor Immune Microenvironment and Prevents Tumor Growth in Lung Adenocarcinoma. Front Oncol 12,873293 (2022).
21. Moreno-Smith, M., Lutgendorf, S.K. & Sood, A.K. Impact of stress on cancer metastasis. Future Oncol 6,1863-1881 (2010).
22. Dai, S. et al. Chronic Stress Promotes Cancer Development. Front Oncol 10,1492 (2020).
READ THIS NEXT
Nourishing Hope: The Vital Role of Nutrition During Cancer Treatment
Cancer is a formidable opponent that affects millions of lives worldwide. While advancements in medical treatments, such as immunotherapy, h
Read MoreCould Curcumin Really Help Cure Cancer?
Cancer is a complex disease that affects millions of people worldwide. While conventional cancer treatments such as chemotherapy, radiation,
Read MoreEGCG and Green Tea Protect Anti-Tumor Immunity
Epigallocatechin gallate (EGCG) is the most abundant catechin in green tea, and one of the most studied polyphenols across the world1.&
Read More